|
12/4/2023 0 Comments Pacemaker failure to capture ekg Sensing is the ability of the pacemaker to detect the heart’s intrinsic electrical activity. This is failure to sense (FTS or under-sensing). Pacing spikes are seen despite normal electrical activity. If you don’t see activity that follows a paced spike then this is failure to capture (FTC)!įigure 4. In other words, it indicates that there is enough energy in the spike to overcome the stimulation threshold. This indicates that the atria or ventricle have been ‘captured’ and depolarization has occurred. If you see a paced spike then you should see a P or QRS immediately following. This is similar to looking for normal sinus rhythm. STEP 2: Is there a P wave or QRS complex following every pacer spike? Too slow = Failure to capture, failure to pace Too fast = Normal response to intrinsic tachycardia, pacemaker-mediated tachycardia, sensor-induced tachycardia, atrial arrhythmias Still, it can help us develop a differential diagnosis when we are dealing with potential pacemaker malfunction. Okay, yes, this is part of our standard approach. The 4 steps are summarized nicely into an algorithm in the above infographic. Now, here are 4 steps that you can add to your regular approach whenever you see a paced ECG. It is important to note that this diagnostic dilemma will often still require the help of our cardiology colleagues. An ECG is a helpful initial test in determining the cause of pacemaker malfunction. The purpose of the following steps is to provide the emergency physician with a simple way to approach pacemaker malfunction. This way you won’t get distracted by a wide QRS following a pacing spike and miss something like ST elevation. It is important to go through a consistent approach when interpreting pacemaker ECGs, ideally the same one you use for non-paced ECGs. delivering the spike to depolarize the myocardium), or sensing. When it malfunctions, the issue is with rate, pacing, capturing (i.e. 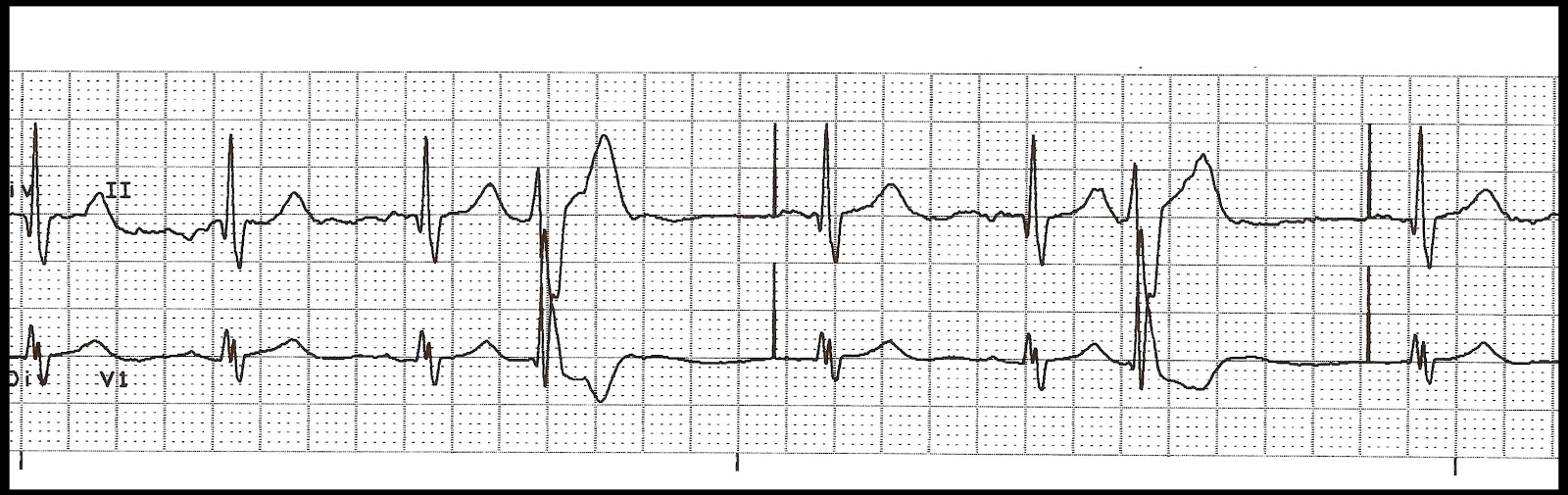
the pacemaker or pulse generator) and a lead or leads. 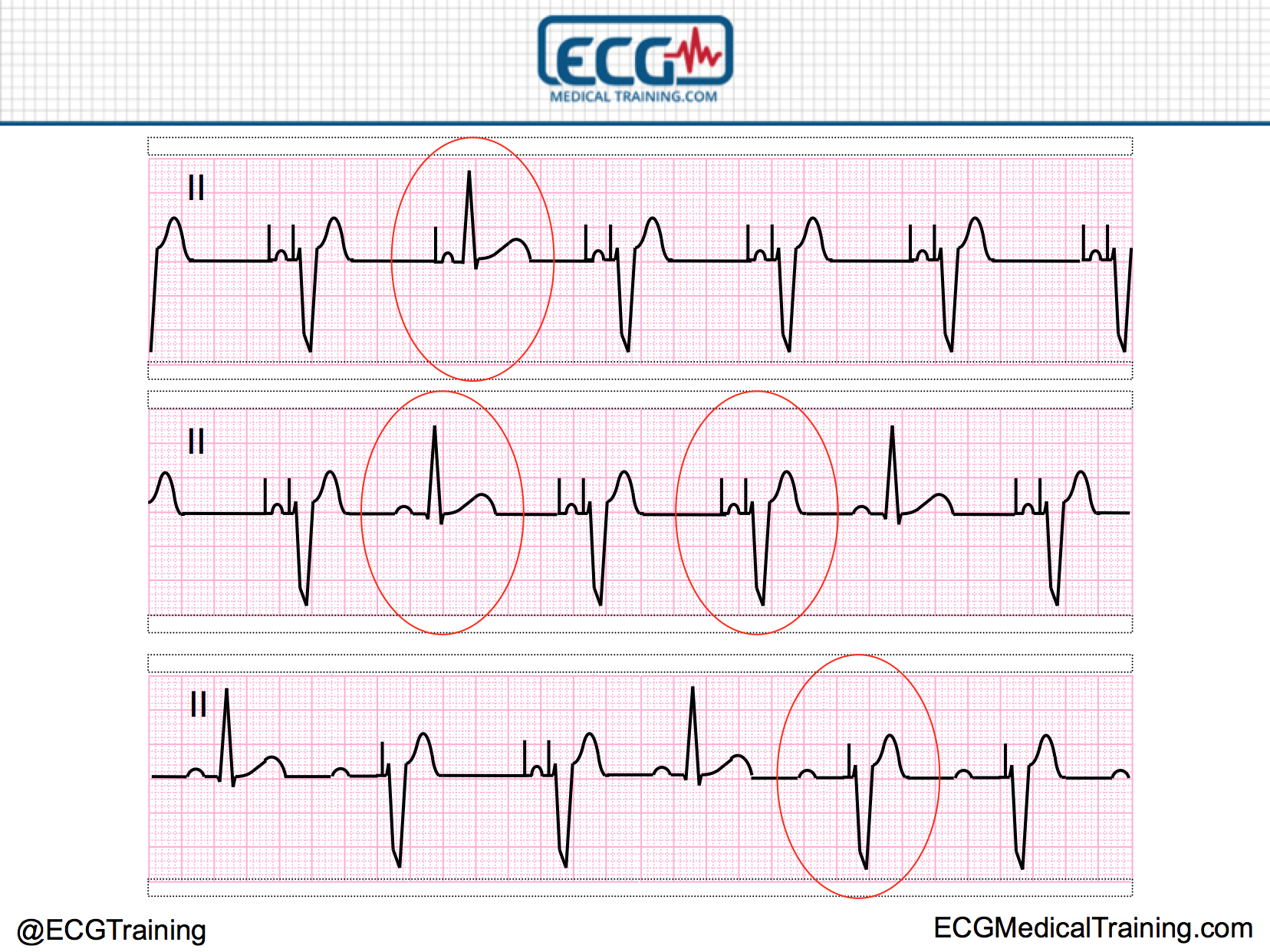
Paced, Fusion, and Capture Beats Approach to a Pacemaker ECGĪ pacemaker consists of a box (i.e. It should be narrower and have a different morphology than your paced beats.įigure 1. Capture beats – the native beat breaks through and is conducted by the ventricle.Fusion beats – the native beat and pacemaker beat fuse, causing an odd hybrid QRS complex.Look carefully in each lead to make sure you’re not missing a subtle paced spike! The majority of permanent pacemakers seen in the ED will have leads in the RV and have a LBBB pattern. If, on the other hand, the lead is in the LV, it will produce a right bundle branch block (RBBB) pattern. If a lead is in the right ventricle (RV), it produces a left bundle branch block (LBBB) pattern on ECG, as the paced beat depolarizes across the myocardium.Since the native rhythm is currently normal, the pacemaker isn’t triggered, and instead sits back and senses the rhythm. For example, a patient who has a pacemaker with a currently-appropriate native rhythm may have an ECG that looks like the one above. This ECG shows normal sinus rhythm, and this does not rule out the presence of a pacemaker. His vitals are stable.ĭoes this person actually have a pacemaker? 
His past medical history is significant for a permanent pacemaker (PPM) that was placed for complete heart block three years ago. The patient is a 68-year-old male with chest pain. It’s Saturday night and you are handed the following ECG. Check out part 1, “ Pacemaker Essentials: What we need to know in the ED” if you haven’t already! If you’d like to download a personal version of the above infographic, click here. Let’s shift our focus to the ECG, and hopefully we’ll discover some pearls to help us with these troublesome devices. Is that pesky pacemaker still causing you trouble? It means well but sometimes it can rub emergency physicians the wrong way. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
